Looking Back Is Looking Forward: The Case of Ebola, COVID-19 and the Future
Nigeria, as well as the rest of the world, is in an unusual time. Never before in modern times have health-related issues moved from the centre-spread of newspapers and from the hidden column health sections to dominate the front page of newspapers and online news platforms, respectively.
PAY ATTENTION: Click “See First” under the “Following” tab to see Legit.ng News on your Facebook News Feed!
This began with the COVID-19 pandemic
When the pandemic broke out in Wuhan, China, in late 2019, the world was largely unprepared for its outbreak. In Nigeria, the situation was similar. It wasn’t until March that a travel ban was issued by the government in a bid to stem the spread of the virus. Since then, more than 179,000 cases have been recorded, with more than 2000 deaths. Despite this seemingly high figure, it still remains one of the lowest figures in the world based on population, thanks largely to the work of the Nigeria Centre for Disease Control (NCDC).
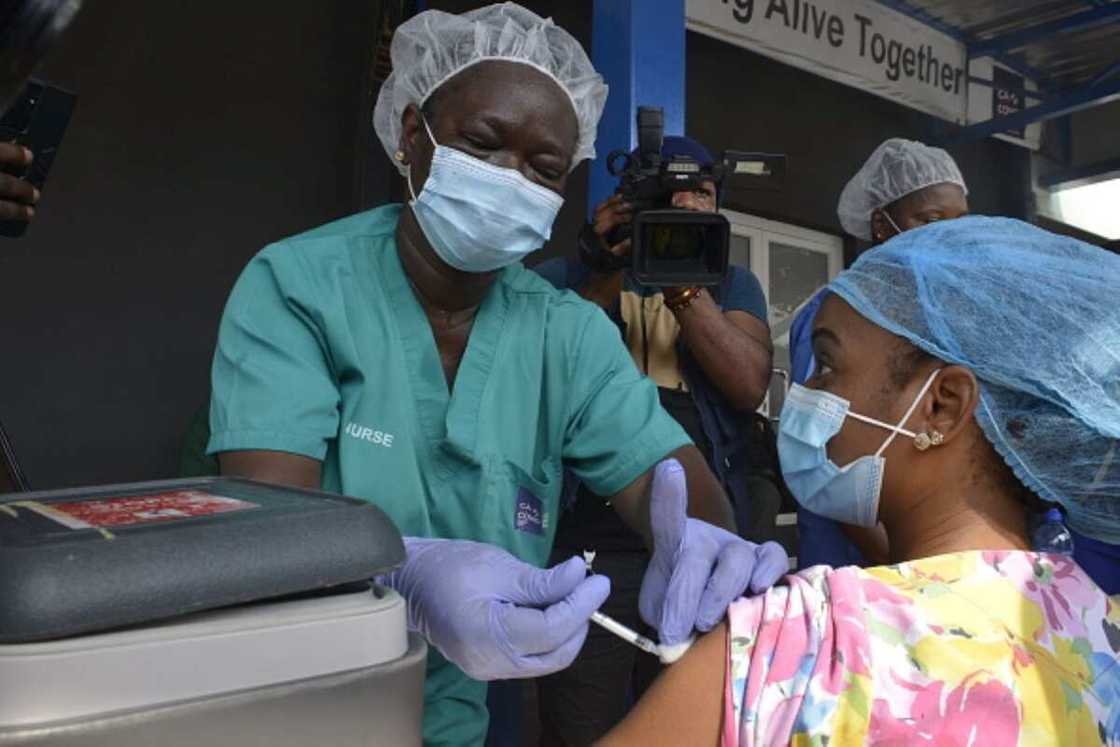
Source: Getty Images
But there is still a lot more to be done. Nigeria was forced to shut its borders and issue a stay-at-home order which adversely affected the economy and raised the unemployment rate to 33 per cent.
As Nigeria is trying to grapple with the effect of the pandemic, which is still ongoing, and the health reports are beginning to move from the front page to the centre-page of newspapers, it is time to consider what Nigeria can do differently when and not if the next viral outbreak comes. To assess this is to take a journey to the past and examine the recent notable outbreak and how it can help shape the future.
Do you have a groundbreaking story you would like us to publish? Please reach us through info@corp.legit.ng!
Looking Back: The case of Ebola
On March 25, 2014, the World Health Organisation confirmed the outbreak of the Ebola Virus in Guinea, Liberia, and Sierra Leone. Four months later, Nigeria recorded its index case when Liberian national Patrick Sawyer flew to Nigeria. Despite caring for his sister, who had the virus in Liberia, and being hospitalised for four days, he lied to the staff at First Consultants Medical Centre that he had not been in contact with anyone with the virus. Dr. Ameyo Adedavoh, however, prevented him from leaving the hospital, a move many credited with helping to mitigate the spread of the virus. Five days later, Sawyer died but not before five health workers from the hospital had been infected.
Despite the seemingly early detection, Dr. Adedavoh was infected with the virus. One Mrs. Ukoh, who was a ward maid at the hospital, was also infected. In all, four health workers who cared for Sawyer contracted the virus and ultimately died.
The federal government of Nigeria announced a N1.9 billion Ebola Intervention Fund to Lagos and Rivers state, where there had been recorded cases of the virus. In August 2014, the Lagos state government announced that the intervention fund promised by the federal government had not been received. This delay might have changed the outcome of the Ebola outbreak if other financial support had not come as confirmed by the state. According to Reuters, Aliko Dangote donated $150 million to curb the spread of the virus, and this was confirmed by the government.
Ultimately, on September 22, 2014, Nigeria officially announced the end of Ebola in the country with 20 cases and eight deaths.
Nigeria’s handling of the Ebola outbreak received a global commendation. The European Centre for Disease Prevention and Control acknowledged the importance of contact tracing and isolation in helping to reduce the spread of the virus. The World health organisation described it as “a piece of world-class epidemiological detective work.” Scientific American concisely describes how Nigeria was able to stop what could have been a rapid spread of if the infectious disease:
“The swift battle was won not only with vigilant disinfecting, port-of-entry screening and rapid isolation but also with boot leather and lots and lots of in-person follow-up visits, completing 18,500 of them to find any new cases of Ebola among a total of 989 identified contacts.”
Perhaps the story might have been different if a key element of the rapid containment of the virus was not provided: Funding. The federal government was accused of not immediately disbursing the promised Ebola intervention fund. Without timely and appropriate funding, the efforts of health workers would have hit a brick wall as contact tracing, and isolation of infected persons would not have been possible.
The Present: Covid-19
Unlike the Ebola outbreak that Nigeria was able to curb quickly, the Covid-19 pandemic spread quickly in Nigeria before the government ultimately announced travel restrictions.
Although the NCDC deployed a Rapid Response team to Lagos and Ogun state, more cases were soon recorded in other states.
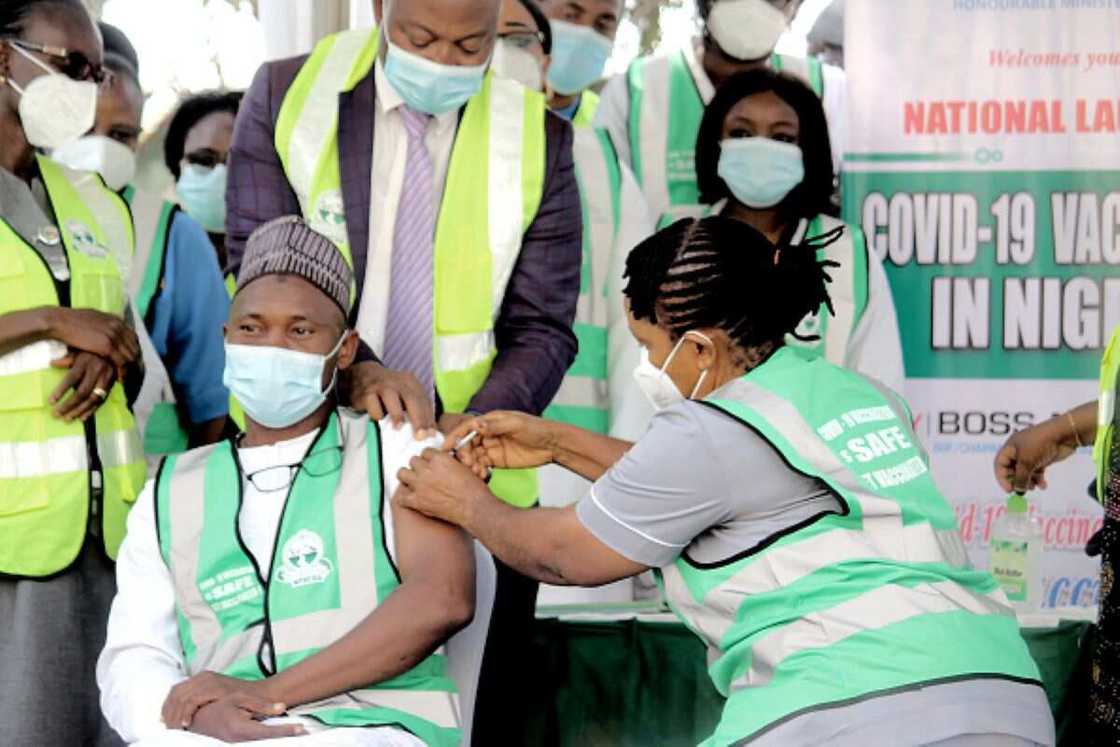
Source: Getty Images
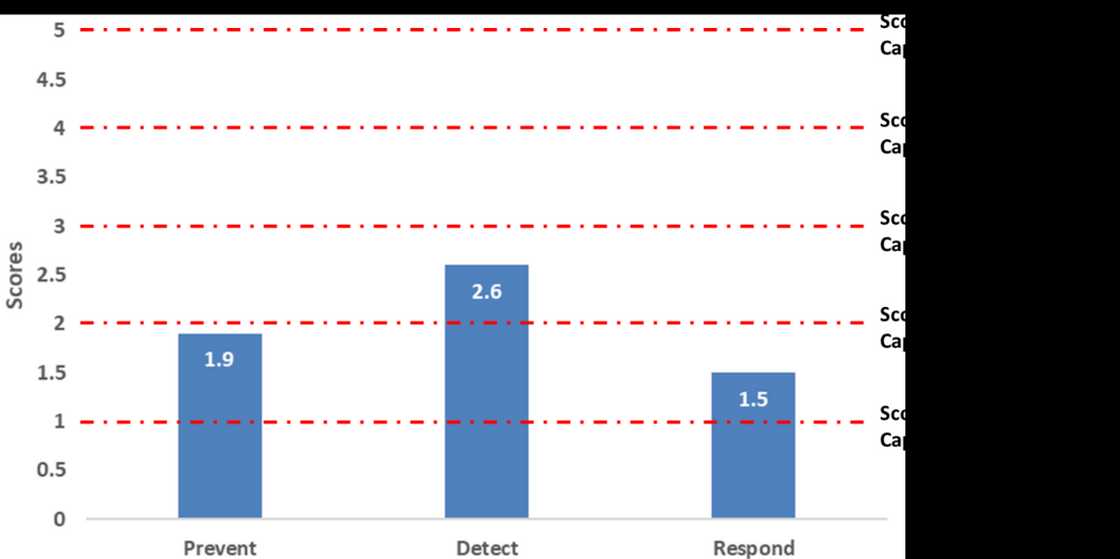
With close to 200,000 confirmed cases and more than 2,000 deaths, why did it seems like Nigeria did not perform well compared to how it managed the Ebola infection? The answer lies in the World Health organisation’s Joint External Evaluation released in 2017 that analysis the preparedness of different countries to respond to public health risk.
While Nigeria performed well in the detect category, which means the country has the ability to discover the existence of a viral outbreak, it performed poorly in the prevent and respond categories.
Source: Facebook
What this shows is that there is a significant disconnect between Nigeria’s ability to detect a health risk and its response to it. This can significantly be bridged through funding.
Funding
On April 27, 2001, heads of state and government of the African Union held a summit in Abuja where they discussed several health issues bedevilling the continent. In the end, they made several commitments with Nigeria, making a 15% budget pledge for the health ministry. 20 years after, Nigeria has failed to actualise its pledge in what has now come to be known as the Abuja Declaration.
Only in 2012 did the country reach a budget peak of 6.2% for the health ministry and has never reached half of its pledge.
Beyond the ministry, several organisations have also continued to contribute to the health sector, particularly in the area of infectious disease. The Health Watch Foundation, for example, is a not-for-profit organisation that “uses informed advocacy and communication to seek better health and access to healthcare in Nigeria.”
This foundation, like others, takes up the task of sensitising Nigerians as well as pushing for policies that would be beneficial to the health sector as a whole. With proper funding, they would reach more (vulnerable) Nigerians and bridge the gap between detection and response to infectious disease.
Looking forward
Covid-19 will not be the last pandemic that Nigeria and the rest of the world will have to face. The World Health Organisation also confirms this and has urged more countries to be prepared. Nigeria’s experience with Ebola should have been an experience for the Covid-19 pandemic as well as for the future, as Dr. Oni Oluseyi puts it.
According to him, policy and funding remain key problems affecting Nigeria’s ability to respond to infectious diseases. While the country learnt a lot from managing the Ebola outbreak, government policies and lack of adequate funding remain central.
He said:
“I’ll say we used the experience of Ebola in managing the Covid-19 pandemic, and we can always use the Covid-19 experience to prepare for the next one. What has always been our problem is leadership and policies. We can be better prepared if the government shows more willpower.
“In the long run, what we need to improve is our data gathering, put more funding into research and take our health sector seriously and invest our people.”
On his part, Mallam Hamzat Lawal, an anti-corruption activist and founder of Follow The Money, a social accountability initiative currently monitoring COVID-19 spending in the country, stated that preparing for the future will depend largely on the nature/kind of the pandemic.
His words:
“We have seen and robustly managed epidemics and outbreaks of diseases such as Ebola, polio, and now COVID-19. However, combating and curbing the spread of these diseases has exposed the weaknesses in our healthcare system and one commonality across the country is the lack of standard healthcare infrastructure and facilities and that is where we need to start from.
“No measure of response and preparation for any pandemic would be enough if the fundamentals i.e healthcare infrastructure and service delivery are subpar.”
Speaking on how the National Primary Health Care Development Agency (NPHCDA) will tackle future pandemics, Yanda Muhammad, spokesman of the agency said:
“Our mandate at the NPHCDA is to ensure the administration of vaccines to all actions in every community in the country, including the hard-to-reach areas. We make sure that the benefits of vaccine to the people is taken to every household across Nigeria.”
Preparing for the future
As we move forward, authorities in Nigeria should be concerned with the functionality of the facilities built or rehabilitated at the peak of the Covid-19 pandemic, so they would not break down.
There should be proper data for planning, comprehensive research in health, investment in manufacturing, and human development.
Nigeria also needs to put its resources together with other African countries to build synergy for breakthroughs in the health sector.
This article was supported by Global Health Advocacy Incubator, A Program of the Campaign for Tobacco-Free Kids, and Vital Strategies.
Source: Legit.ng



